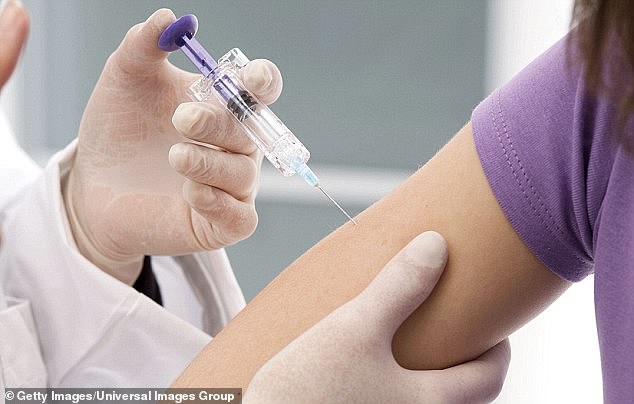
- Researchers studied women who moderate or severe precancerous lesions
- Some received a vaccine, which injects a protein that triggers the immune system to attack the lesions
- About 36 percent of women with the most severe lesions saw them disappear compared to the placebo group
- When followed up after 2.5 years, women who received the vaccine were more likely to be completely clear of the underlying HPV infection
A new vaccine cleared up HPV infections in women who had precancerous lesions on their cervix – preventing it from developing, according to a new study.
The shot injects a protein that triggers the immune system to attack precancerous changes in the cervix, specifically lesions known as CIN.
About one-third of women who had the most severe lesions had them clear up as well as the HPV infection itself.
The team, from Michigan Medicine, says the vaccine is safer, cheaper and easier than surgery to remove the lesions and could be a new way of preventing precancerous changes in the cervix from developing into disease.
A new study from Michigan Medicine found that a new vaccine not only cleared up precancerous lesions in women caused by HPV, but the infection itself (file image)
HPV, short for Human papillomavirus, is the most common STI in the US, affecting around 79 million people. It has been linked to numerous cancers – including prostate, throat, head and neck, rectum and cervical cancer.
Since the HPV vaccine was introduced in 2006, 79 countries and territories have implemented a publicly funded national HPV vaccination program.
In the US, the vaccine is offered in two or three doses over the course of six months to girls who are between 11 and 12, with a catch-up series recommended no later than age 26.
In the UK, all girls between ages 12 and 18 are offered free vaccination against HPV over six to 12 months, as well as 12- and 13-year-old boys.
Lead author Dr Diane Harper, a professor of family medicine and obstetrics and gynecology at Michigan Medicine, said the vaccine in the new study is different than the Gardasil vaccine, which prevents HPV infection.
The new shot, known as Tipapkinogen Sovacivec, clears tissue already infected with HPV.
CIN lesions are split into three categories: CIN 1 lesions generally go away without treatment, CIN 2 lesions can go away on their own but can also progress, and CIN 3 lesions are the most severe.
About half of the severe lesions will progress to cancer within 30 years.
‘We have no way to determine which women with CIN 3 will progress to cancer and which women will not,’ Dr Harper said. ‘So we treat all women with CIN 2 or 3 as if they are likely to develop cancer.’
For the study, published in Gynecologic Oncology, the team studied 200 women who had moderate or severe lesions.
About 130 participants were randomly selected to receive the vaccine while the rest received a placebo.
Researchers found that the women who were administered the vaccine were two times more likely to see their lesions disappear than the placebo group.
They found even more surprising results in the group with the most severe lesions. About 36 percent who got the vaccine saw their lesions disappear, but none in the placebo group did.
The women were then followed up with for another 2.5 years. The team found that those who received vaccine were more likely to be completely clear of HPV than the placebo group.
‘There are very few products trying to cure women who already have an HPV infection,’ said Dr Harper.
‘It’s very exciting. This is the first time we’ve seen something with this success rate that is relatively easy to implement.’
Treatment for these lesions usually involves removing a piece of the cervix, but complication include scarring and a shortened cervix, which could lead to problems when delivering a child.
‘The surgical procedure removes all the tissue that is headed towards cancer, but it doesn’t remove all the HPV. You’re not home-free. You still have HPV,’ said Dr Harper.
‘The vaccine actually treats the cause of the disease, which is HPV.’
Source: Dailymail.
 Based on +200
reviews
Based on +200
reviews